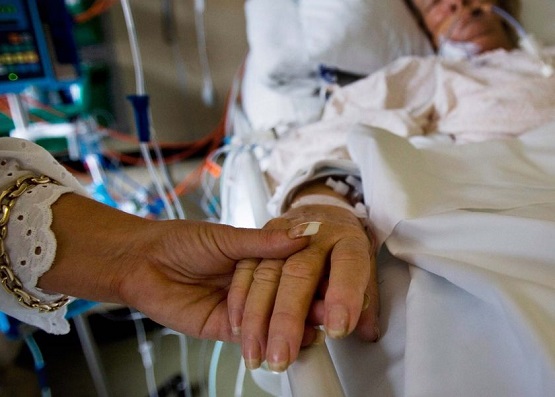
There are no easy answers in a healthcare crisis, especially when the demand for certain life-saving or sustaining treatments become greater than its availability.
Justice and equality (non-maleficence) require us to provide healthcare for everyone who will benefit and yet if the availability of certain resources are limited then decisions are made which are often unjust and lack equality.
People with disabilities and the elderly are considered to be more likely to die from Covid-19 and therefore they may be denied life-saving or sustaining treatments to enable a person who is viewed as more likely to survive to receive treatment.
In a utilitarian sense, this approach seems rational, but when considering justice and equality these measures fail because they are based on selecting who will live and who will die based on personal beliefs that are often linked to negative or discriminatory attitudes or ideologies concerning people requiring different care.
A situation where a person chooses not to receive treatment because they have accepted that they are unlikely to survive or decided that the treatment outweighs the possible benefits is different because no one is imposing the withholding of treatment.
A situation where a person is truly dying and the treatment is futile, whether that person is 30 or 90 years of age is different. There is no societal obligation to provide treatment that lacks benefit or is medically futile. In this circumstance the person is not deemed futile but the treatment is futile.
People with disabilities are genuinely fear that they will not be considered “worthy” for treatment, even when the benefit of the treatment is recovery. Further to that, some people with disabilities already require ventilator support to live. Should these people be denied ventilator support or have it withdrawn against their needs and wishes simply because another person requires a ventilator?
REACH PRO-LIFE PEOPLE WORLDWIDE! Advertise with LifeNews to reach hundreds of thousands of pro-life readers every week. Contact us today.
Pandemic palliative care: beyond ventilators and saving lives.
The CMAJ (March 31) published a protocol on the care of Covid-19 patients who are being withheld or withdrawn from treatment titled: Pandemic palliative care: beyond ventilators and saving lives. The authors of the protocol include Dr James Downar, the former chair of the Dying with Dignity Physician Advisory Committee and Dr Sandy Buchman, President of the Canadian Medical Association.
Read: Euthanasia doctor developed Ontario Covid-19 triage guidelines (Link).
The authors are asking for a response to the protocol. This is my assessment.
The protocol claims to be based on fairness and equality, but actually institutionalizes the inequality and injustice that lead to people with disabilities and other vulnerable groups being selected for death based on negative and discriminatory attitudes.
The protocol states:
Many people already have advance care plans that stipulate that comfort measures are to be used if they become seriously ill. Other patients who are intubated and receiving mechanical ventilation but are not improving clinically will be extubated. A third group of patients may be denied ventilation because of resource scarcity.
This statement tells us not to have blanket statements in our healthcare directive requiring comfort measures only. Certain medical conditions may lead to recovery with treatment, but with the above wording, no treatment will be provided.
This statement is also unethical. To withdraw a ventilator requires consent from the patient or the power of attorney. Decisions to withdraw treatment require consent in the same manner as decisions to provide treatment.
People with disabilities who require a ventilator fear that decisions will be made to extubate them because their health condition is not clinically improving. People with disabilities may not “clinically improve” not because they are treatment resistant but because of the nature of the disability. It is discrimination to deny treatment based on disability.
The protocol states that when a person is denied treatment that they must be provided palliative care. The authors state that they are not abandoning the patient when they provide palliative care and yet the triage system has already abandoned the patient.
The protocol leads to an abuse of the ethical use of palliative sedation.
Palliative sedation or terminal sedation is properly used for a patient who has symptoms that cannot be effectively alleviated in any other way. For instance, a person who is living with Neuropathic pain may only be effectively relieved of the pain through sedation. The authors of this protocol are proposing the use of sedation as a means of causing death, instead of (MAiD) euthanasia which is legal in Canada. The protocol states:
In our opinion, palliative sedation is preferable to medical assistance in dying (MAiD) for patients with severe respiratory failure caused by SARS-CoV-2, given the 10-day reflection period, number of witnesses and assessors required, and the current requirement for full capacity to determine eligibility for MAiD.
When analyzing euthanasia data from the Netherlands and Belgium you will notice a significant number of “assisted deaths without explicit request” that occur on a yearly basis. This protocol is endorsing the same procedures that are done in the Netherlands and Belgium to circumvent the euthanasia law. Downar is well aware that he is advocating for intentional acts to cause death. In 2014 Downar participated in the study: Characteristics of Belgian “life ending acts without explicit request.”
The protocol changes the ideology of palliative care. The concept of palliative care is to provide pain and symptom relief when a person is dying, to palliate the symptoms but never to hasten death. The protocol is suggesting that palliative care can replace active treatment, even when treatment may lead to recovery. So palliative care becomes a way of providing a comfortable death for people who have been medically abandoned.
The protocol claims that it will lead to greater equity. The protocol acknowledges that people who live with mental illness or other conditions face substantial challenges to receiving healthcare and they conclude that: “Palliative care thus becomes the compassionate option to counterbalance this inequality.”
Palliative care is better than “sending them home to die” and to not palliate symptoms is to abandon the patient again. Nonetheless, this protocol institutionalizes the inequality and injustice. The protocol states that you must be kept comfortable as we abandon you. But it doesn’t stop there, the protocol advocates for the abuse of the use of “palliative sedation” meaning, we will not only palliative your symptoms, but in certain circumstances we will end your life without your explicit consent.
LifeNews.com Note: Alex Schadenberg is the executive director of the Euthanasia Prevention Coalition and you can read his blog here.