A Texas court has stepped in to stop a Fort Worth hospital from pulling the plug on a 10-month-old baby without her mother’s consent.
Cook Children’s Fort Worth was slated to pull the plug on little Tinslee Lewis against her mother’s will. But pro-life advocates helped Tinslee’s mother fight for her in court.
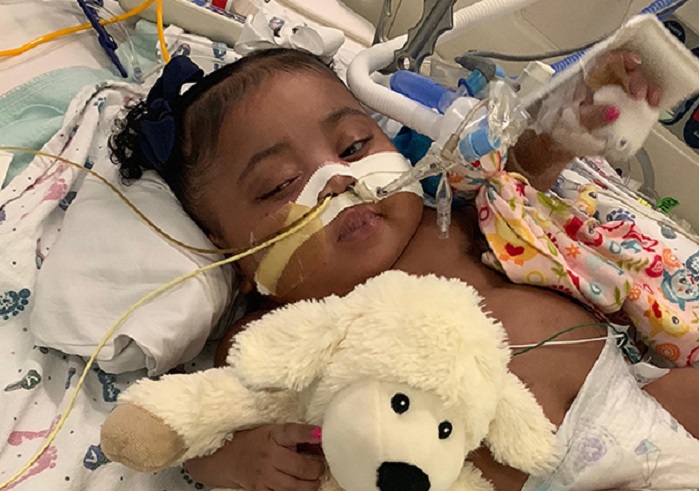
Baby Tinslee is a 9-month-old girl with congenital heart disease and is breathing with the assistance of a ventilator. She is sedated but conscious. Cook Children’s Fort Worth Hospital informed Tinslee’s mother, Trinity, on October 31 that they would pull the plug on her daughter against her directive in 10 days, scheduling her to die on Sunday.
The family and hospital have been in a tenuous legal battle ever since.
Thankfully, yesterday, Justice Sandee Marion, Chief Justice of the 4th Court of Appeals, granted more time for Baby Tinslee Lewis before she would issue a formal ruling on a temporary injunction.
A temporary injunction would prevent Cook Children’s Hospital in Fort Worth from pulling the plug under the Texas 10-Day Rule on the 10-month-old against her mother’s will. Tinslee is now protected until January 2, 2020, from euthanasia as the family continues to work with Texas Right to Life and Protect TX Fragile Kids to seek another hospital that would care for her.
“I’m so grateful that my baby won more time today,” said Trinity Lewis, Tinslee’s mother. “A month ago, I thought I was going to lose my baby to this 10-Day Rule. But now we have more time to find a new hospital that will care for her and we want to stop this from happening to any other parent ever again.”
Texas Right to Life told LifeNews.com that it is “glad that the judge granted more time for Baby Tinslee. Tinslee’s right to due process and her Right to Life are both at stake of being robbed by the deadly 10-Day Rule. We will continue working with Trinity Lewis until Baby Tinslee is safe, and will keep fighting this anti-Life law, which Texas Attorney General Ken Paxton deemed unconstitutional in his amicus brief defending Tinslee.”
“However, unless Governor Greg Abbott calls a special session to repeal the 10-Day Rule, Tinslee Lewis will not be the last patient victimized by this law. Texans who want to protect patients like Tinslee should contact their state legislators at (512) 463-4630,” it added.
The 10-Day Rule is a provision in the Texas Advance Directives Act (Chapter 166.046 of the Texas Health & Safety Code) that allows a hospital ethics committee to withdraw basic life-sustaining care, like a ventilator or dialysis, from a patient against his expressed will, his advance directive, or the instruction of his surrogate decision-maker. Ten days after informing the patient or surrogate of the committee’s decision, the hospital can remove basic life-sustaining care from a patient.
Click here to sign up for pro-life news alerts from LifeNews.com
Committees can withdraw care for any reason and the patient cannot appeal the decision. Even if the patient is conscious, coherent, and actively requests to stay alive, the 10-Day-Rule allows the hospital to overrule the patient’s will.
Attorney Wesley Smith, a noted writer and author on end of life issues, testified in favor of legislation to stop the rule. During his testimony he broke down the problems with the 10-day rule:
In Texas, patient autonomy is essentially a one-way street. Here, if a doctor disagrees with the patient’s decision to maintain life—and the patient or family refuses to permit the life-extending treatment to be withdrawn—the doctor can take the controversy to the hospital bioethics committee for a quasi-judicial hearing and binding ultimate ruling.
If the committee agrees with the doctor, the patient or family has only 10-days within which to find an alternative source of treatment and arrange a transfer. If they can’t, the life-extending treatment can be terminated over the patient or surrogate’s objection—meaning the patient will be forced into a death at a time when life could have been maintained.
To fully comprehend the unjust nature of Texas law in this regard, realize that these “futile care” or “inappropriate care” decisions do not terminate treatment because it won’t work, but because it does. It is keeping the patient alive when the doctor/bioethics committee thinks the patient should die.
This isn’t an objective medical determination, but a subjective value judgment. And given the subjective nature of such decision making—which involves the question of whether the among of suffering the intervention may cause outweighs the desire to maintain life—the law should give the ultimate power to decide such questions to patients, families, and duly appointed surrogates who know the patient most intimately, not to bioethics committee members who are strangers to the patient.