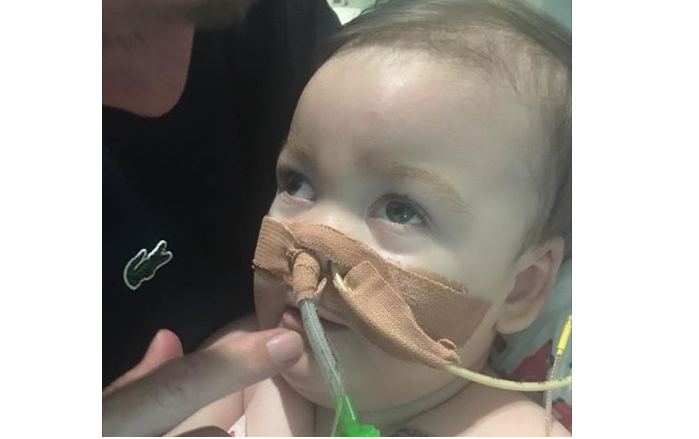
Defending the UK High Court’s order allowing Alder Hay Children’s Hospital to withdraw life support from Baby Alfie Evans and refusing to even allow his parents to take him home, Dr. Ranj Singh of the UK National Health Service was quoted saying, “This is not the killing of a child – this is redirecting care to make them more comfortable.”
Although this callous statement suggests an economic motive, I believe the real problem is a fundamental shift in legal and medical ethics that started in the U.S. in 1976 with the Karen Quinlan case.
Karen was a 21-year- old woman whose parents wanted to remove her ventilator after she did not wake up after losing consciousness after a party. The doctors disagreed but the California Supreme Court upheld parents’ decision by stating:
“No compelling interest of the state could compel Karen to endure the unendurable, only to vegetate a few measurable months with no realistic possibility of returning to any semblance of cognitive or sapient state,” then-Chief Justice Richard Hughes wrote. (Emphasis added)
Ironically, Karen did not stop breathing and lived 9 more years with a feeding tube and basic care. But Karen’s case set the stage for the so-called “right to die” movement, “living wills” with removal of feedings, and eventually the current assisted suicide/euthanasia movement.
Unfortunately, Baby Alfie and his parents are just the latest casualties of an emerging legal/medical/popular mindset that some people are better off dead. To make matters worse, Baby Alfie’s case–like the similar Baby Charlie Gard case in the UK last year–are perhaps intended to become examples to discourage other parents (or families) from challenging doctors, hospitals and courts on mandatory withdrawal of treatment decisions.
WHAT HAPPENED TO BABY ALFIE AND COULD THIS HAPPEN HERE IN THE US?
Baby Alfie Evans was born in the UK on May 9, 2016 and apparently healthy. His parents became concerned when he missed the developmental milestones that most babies achieve in their first 7 months and started making “jerking, seizure-life movements.”
In December 2016, he caught a chest infection that caused seizures and was placed on a ventilator at Alder Hey Children’s Hospital in Liverpool. Despite the doctors’ dire predictions, Alfie started breathing on his own but caught another chest infection and seizures and went back on a ventilator.
Without having a definitive diagnosis, after a year and Baby Alfie in what his doctors called a “semi-vegetative” state, the hospital and doctors wanted to remove his ventilator. But Alfie’s parents fought back.
The hospital took the case to the British High Court, stating that “further treatment” for Alfie was “not in his best interests” as well as “unkind and inhumane.”
After many failed court appeals by the parents and even help from Pope Francis and an Italian hospital ready to take the baby, the hospital remained intractable and Alfie was not even allowed to go home with his parents. The ventilator was removed but, contrary to the doctors’ predictions, Alfie continued to breathe on his own for five more days before finally dying.
I watched the tragedy of Baby Alfie from afar with a lot of alarm as well as personal sadness.
I first became aware of medical discrimination against babies with mental disabilities in 1982 with the “Baby Doe” case. Baby Doe was born in Indiana with Down syndrome and a correctable congenital defect in his throat that makes eating food orally impossible. But his parents refused surgery.
The case went to court but the judge ruled in favor of his parents. The parents also refused all offers of adoption.
Baby Doe died from starvation and dehydration while lawyers were still appealing his case. Tragically, Baby Doe did not even receive simple intravenous fluids to keep him alive until his appeals were finished. Many of us who spoke out about Baby Doe’s right to treatment were accused of being “mean” to his parents.
When my daughter Karen was born just after Baby Doe died and also with Down syndrome as well as a treatable heart defect, I was offered the “choice” of refusing heart surgery for her and “letting” her die. However, even after I insisted on the surgery, I found out that one doctor made her a Do Not Resuscitate behind my back and I was told by others-even other health care professionals like myself-things like “People like you shouldn’t be saddled with a child like that!”
I became so fearful that at one point I slept on the floor under my daughter’s crib during an overnight hospitalization for a test.
It was devastating when Karen died from sudden complications of pneumonia at 5 ½ months but I will never regret fighting for her right to be treated the same as other children with her heart defect.
With Baby Simon Crosier who was born with Trisomy 18 and a heart defect in 2010, his parents begged for help when Simon started deteriorating. They did not know that the hospital had made their baby a Do Not Resuscitate and was being given only “comfort feeds” due to a secret futility policy. They had to helplessly watch as Simon died in their arms. The later Simon’s Law bill they helped write to prevent other outrageous secret futility guidelines in hospitals continues to sit in a Missouri legislative committee but hopefully it will get to the House floor this session. (Simon’s Law was passed in Kansas in 2017.)
PARENTAL DECISION-MAKING
The usual standard for parental decision-making in the U,S. has been:
“Medical caretakers have an ethical and legal duty to advocate for the best interests of the child when parental decisions are potentially dangerous to the child’s health, imprudent, neglectful, or abusive. As a general rule, medical caretakers and others should challenge parental decisions when those decisions place the child at significant risk of serious harm.” (Emphasis added)
But, after Baby Doe starved to death, medical groups fought the proposed Baby Doe Regulations intended to protect such children with disabilities as too restrictive. For example, the American Medical Association endorsed the quality of life standard prior to the Baby Doe case:
“In the making of decisions for the treatment of seriously deformed newborns or persons who are severely deteriorated victims of injury, illness, or advanced age, quality of life is a factor to be considered in determining what is best for the individual.
In caring for defective infants the advice and judgment of the physician should be readily available, but the decision as to whether to treat a severely defective infant and exert maximal efforts to sustain life should be the choice of the parents.” (Emphasis added)
But at a pediatric ethics conference in 1994, I was shocked by a workshop where the focus was on how to convince parents to refuse or withdraw treatment from seriously disabled or dying children. One speaker/lawyer was even applauded when he suggested that parents who refused to withdraw treatment like feeding tubes from their “vegetative” children were being “cruel” and even “abusive” by not “allowing” their children to die. He also said that judges would be most likely to side with the doctors and/or ethics committee if such cases went to court.
Over the years and unknown to most of the public, many ethicists still refuse to concede this “choice” of a right to continue treatment and instead have developed a new theory that doctors cannot be forced to provide “inappropriate” or “futile” care to patients of any age. This theory evolved into “futile care” policies at hospitals in Houston, Des Moines, California and other areas. Even Catholic hospitals have been involved.
And now, as Baby Simon’s parents and I have unfortunately found, such decisions are sometimes made without even notifying us. This must change with not only legislation like Simon’s Law but also a change of attitude towards these little ones.
CONCLUSION
While there are situations where a family or patient might unreasonably demand truly medically futile, the decision to deliberately end the life of a person because he or she is deemed to have little or no “quality of life” should never be made.
The terrible ordeal that Baby Alfie and his parents went through sparked tremendous outrage around the world, especially over the callous treatment of his obviously loving parents.
This was inhuman, not “humane” and we must continue the fight to demand truly ethical, caring and nondiscriminatory healthcare, especially for the youngest among us.
LifeNews Note: Nancy Valko, a registered nurse from St. Louis, is a spokeswoman for the National Association of Pro Life Nurses. This appeared at Nancy’s blog and is reposted with permission.