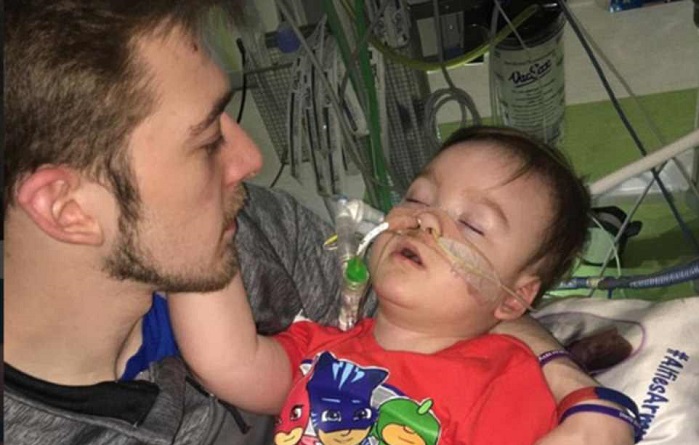
On April 23, 2018, Alfie Evans, who may have been suffering from some form of mitochondrial disorder, had his ventilator removed by the doctors at Alder Hey Children’s Hospital in the UK. Not much is known about Alfie’s medical problem, it is known that it is a neurodegenerative disorder and has no known cure. In December 2017, Bambino Gesu, a respected children’s hospital in Rome offered to accept the transfer of the toddler, yet the doctors at Alder Hey refused.
This is when the parents, Tom Evans and Kate James, begun their fight to have Alfie released to their custody and transferred. Yet time and again, the British and European Union courts ruled against Mr. Evans and Ms. James. Italy even went so far as to grant Alfie citizenship, but it did not influence the courts one iota and Alfie was to remain in the UK. On April 28, Alfie passed away, ending the contentious legal struggle between Alder Hey and Alfie’s parents. Nonetheless, it left many questions for bioethicists to consider.
It became obvious that when it came to end-of-life care, British law was woefully insufficient in protecting the right of the patient to have the ability to transfer to another medical facility that may wish to continue treatment. This reality, of course, begs the question; why is it necessary to have transfer provisions protected under the law especially if the patient will imminently die?
One of the issues to consider is that the law needs to strike a balance between the rights of the patient and the rights of the doctor in order to prevent any form of tyranny whether it be some form of medical tyranny by the doctors who impose their will against the wishes of the patient or some form of patient tyranny against the conscience of the doctor. Horror stories can arise from either scenario. In fact, when it came to the Alfie Evans case one British medical organization called what the doctors were doing to keep Alfie in the UK a form of tyranny.[i]
As mentioned above, a situation where the patient becomes tyrannical over medical care is unethical as well, since the vast majority of patients simply do not have any medical expertise of any sort. If patients are able to direct medical care by forcing doctors to act against their conscience then situations would inevitably arise where doctors would be forced to give treatment that may be contrary to the bodily health of the patient.
Consider the following from St. John Paul II,
To refuse to take part in committing an injustice is not only a moral duty; it is also a basic human right. Were this not so, the human person would be forced to perform an action intrinsically incompatible with human dignity, and in this way human freedom itself, the authentic meaning and purpose of which are found in its orientation to the true and the good, would be radically compromised. What is at stake, therefore, is an essential right which, precisely as such, should be acknowledged and protected by civil law. In this sense, the opportunity to refuse to take part in the phases of consultation, preparation and execution of these acts against life should be guaranteed to physicians, health-care personnel, and directors of hospitals, clinics and convalescent facilities. Those who have recourse to conscientious objection must be protected not only from legal penalties but also from any negative effects on the legal, disciplinary, financial and professional plane.[ii]
It is quite clear that St. John Paul II is arguing that the conscience of the doctor ought to be protected from unjust coercion and that civil law ought to protect this right of the doctor. It is also clear that St. John Paul II also stated that, “The choice of euthanasia becomes more serious when it takes the form of a murder committed by others on a person who has in no way requested it and who has never consented to it. The height of arbitrariness and injustice is reached when certain people, such as physicians or legislators, arrogate to themselves the power to decide who ought to live and who ought to die.”[iii] Here one can readily understand that the doctor does not have the right to arbitrarily judge who has the right to live or die, so the doctor certainly does not have an absolute right. This is further clarified in light of Catholic teaching on extraordinary care, “Discontinuing medical procedures that are burdensome, dangerous, extraordinary, or disproportionate to the expected outcome can be legitimate; it is the refusal of “over-zealous” treatment. Here one does not will to cause death; one’s inability to impede it is merely accepted. The decisions should be made by the patient if he is competent and able or, if not, by those legally entitled to act for the patient, whose reasonable will and legitimate interests must always be respected.”[iv] Here again, one can see that the doctor does not have absolute power over the patient. Extraordinary care, those heroic measures such as experimental therapies, or very risky surgical procedures, is a decision that the patient, or the patient’s surrogate, must decide upon. As a result, the decision implies a right of the patient. In the context of health-care decisions, rights of one imply a duty upon another, the patient has the right to make this decision and the doctor is duty bound not to enforce his will upon the patient.
Follow LifeNews.com on Instagram for pro-life pictures and the latest pro-life news.
This gets to the very core of the idea of the civil law protecting the ability to transfer from one facility to another when a disagreement arises. Doctors, while they are medical experts, can err from time to time on a diagnosis. This is why people are urged to get a second opinion. Even doctors can disagree on what might be the best care for a patient and even the patient can disagree with the doctor on what the best course of action may be. When disagreement occurs, it is important that the ability to transfer can take place and that this ability to transfer be protected under the law. The transfer helps to balance both the rights of the patient and the medical doctors. If another hospital believes that a patient has been misdiagnosed or is not receiving the kind of care that should be given to the patient, then the patient should be transferred. This follows the principle of the safer course which basically asserts that one ought to err on the side of caution. So, in the instance when a disagreement between doctor and patient occurs, the law recognizes that the patient has the ability to transfer and the doctor and medical facility have the duty to let that patient transfer if another hospital is willing to let him. This recognizes that the law is erring on the side of life, just in case the original doctor’s diagnosis was incorrect.
Unfortunately, it was painfully obvious that this ability to transfer to another medical facility was not protected under British law when it came to the Alfie Evans case. While there were many questions in light of the palliative care that Alfie Evans received (such as why did they wait so long to give him oxygen?), the vast majority of pro-life advocates were absolutely perplexed as to why Adler Hey would not greenlight the transfer. It showed a reckless disregard for patient’s rights. It was evident that Alfie’s parents did not agree with the care at Alder Hey and the Italian hospital, Bambino Gesu, was more than willing to take young Alfie. Alder Hey had a moral obligation to respect this right even if they disagreed with the parents since the moral right resided with them as the surrogate decision makers for young Alfie.
In his most recent opinion piece,[v] Professor Carter Snead, who teaches at the University of Notre Dame, argues that the UK needs to change its laws to help better ensure that parents who have a disabled child have the freedom to help their child with the best care they see fit. Enshrining the ability to transfer could be a step in the right direction for the UK and any other jurisdiction that does not protect this right of the patient or of the parents of a patient who is a minor. While the legal protections of a transfer are not a guarantee that transfer will happen, it does protect the right of the patient to seek moral medical care elsewhere when disagreement occurs. Tragically, it is too late for Alfie Evans, but if a law were in place protecting this ability, Mr. Evans and Ms. James would not have had to fight so many unjust and notorious legal battles and Alfie would have been transferred to Rome without so much as a fuss.
In order to better protect a Culture of Life more needs to be done to ensure this type of legislation passes in the future so as to safeguard from another tragic situation like that of Alfie Evans.
__________________________
[ii] Evangelium Vitae, no. 74.
[iii] Evangelium Vitae, no. 66.
[iv] Catechism of the Catholic Church, no. 2278.
[v] See https://www.cnn.com/2018/04/29/opinions/alfie-evans-opinion-snead/index.html
LifeNews Note: Joe Kral, M.A., is the President of the Society of St. Sebastian and Editor-in-Chief of the Journal of Bioethics in Law & Culture Quarterly.